Some things cannot be explained by conventional thinking. Here is one example. Earlier I reviewed new Nature paper discussing the beneficial role of allo-IgG in cancer therapy.
This time, however, another team of scientists reported in the same issue of Nature that B cells and IgA secreting cell in particular, suppress effectiveness of platinum-based anti-cancer compounds, such as oxaliplatin.
The authors, led by Michael Karin at the University of California, San Diego (UCSD), analyzed oxaliplatin's effect in tumor bearing mice. Surprisingly, B cell deficient mice showed significant synergy with oxaliplatin.
This beneficial effect of B cell ablation on anti-cancer effect of oxaliplatin was CD8 T cell-dependent.
Next, the authors showed that inhibition of oxaliplatin-induced anti-cancer effect was related to TGF-beta signaling in B cells and their differentiation into IgA producing cells.
Furthermore, the authors showed that B cell-specific expression of IL-10 and PD-L1/2 contributed to cancer resistance towards oxaliplatin.
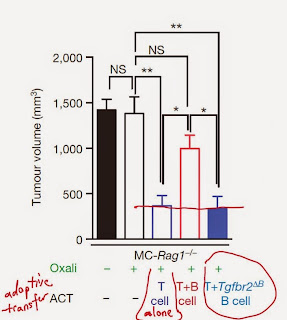
Finally, the authors showed that adoptive co-transfer of B cells with T cells induced cancer resistance to oxaliplatin's treatment via TGF-beta signaling.
In summary, these results suggest that initial anti-cancer action of oxaliplatin primes B cells to develop into IgA secreting cells and to inhibit CD8 T cell's anti-cancer effector function via IL-10 and PD-L1/2 signalling.
It is not clear whether IgA secretion per se has any inhibitory role. It appears that oxaliplatin activates or amplifies pathways towards IgA differentiation that is inhibitory to CTL functions. Does oxaliplatin action mimics gut immune environment? This fact requires further investigation to understand its mode of action. It could have a separate usefulness for oral vaccine formulations.
David Usharauli




No comments:
Post a Comment